What do I do now?
One of the questions parents ask about a lot is what happens if my baby has an allergic reaction during weaning? What next steps should parents/carers take next. This blog aims to answer this question with the help of Lydia Collins-Hussey, The Milk Allergy Dietitian.
Disclaimer: The content in this blog should not replace individual medical advice and is for informational purposes only. In the first instance, if you are unsure if your baby has had an allergic reaction, you should always speak with your Health Care Professional (HCP).
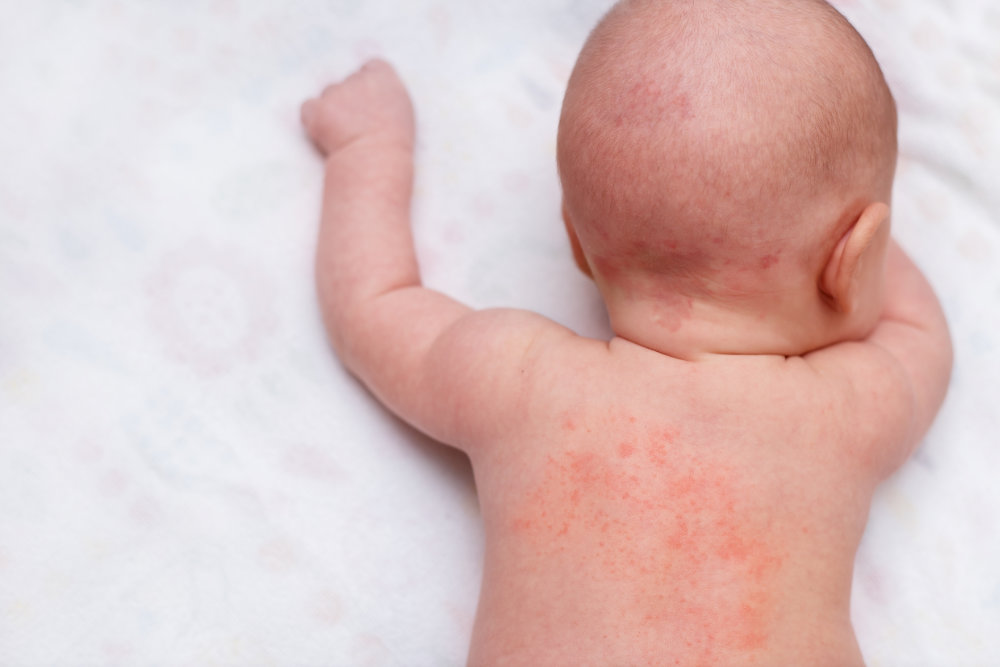
What is an allergic reaction and when is it not one?
There are two types of allergic reactions;
- IgE mediated reactions, (these happen quickly) and
- Non IgE mediated reactions (these are delayed)
Let’s summarise further…
| IgE mediated allergy (immediate) | Non IgE mediated allergy (delayed) |
| Symptoms typically develop within seconds/minutes up to 2 hours after ingesting the culprit food. Example of symptoms include red blotchy rash or hives, lip or eye swelling and in severe cases breathing difficulties or those affecting circulation (floppiness and tiredness) (this list is not exhaustive) | Symptoms develop after 2 hours up to 72 hours after ingesting the culprit food. Example of symptoms: blood or mucus stools, reflux, diarrhoea, constipation, colic (this list is not exhaustive) |
| Easier to diagnose | Harder to diagnose as symptoms can overlap with common symptoms that can occur early in life (e.g reflux) |
| There are tests that can be conducted alongside a clinical history and include skin prick test and specific IgE blood test. | Unfortunately, there is no test for this type of allergy. Diagnosis is an exclusion diet for a period of 2-4 weeks with a reintroduction challenge to confirm/exclude. |
Both these reactions involve our immune system. A non IgE mediated allergy often gets confused with an intolerance but there is a difference, an intolerance typically involves just gut symptoms and does not involve the immune system. The most common example is lactose intolerance which is where symptoms present due to the sugar in milk. When we have an allergic reaction, it is to the protein in that food.
Contact irritation is not a true allergy
Contact irritation can be common in babies and children particularly with sensitive skin or eczema. Contact irritation presents where the food has touched, commonly around baby’s mouth or hands. The rash can appear quickly but also disappear quickly.
Contact irritation typically presents to foods high in histamine such as tomato, banana and aubergine and also to spices, citrus and berry fruits. In these cases, the rash red is localised to around the mouth or hands and often baby is not irritated or aware of it. This is not a food allergy, and these foods don’t usually have to be avoided. Applying a barrier cream around baby’s mouth can help to reduce the rash from developing.
So how do you know if it is irritation or an allergy rash?
Babies can present with rashes for many different reasons, including a dribble rash, viral or fever, or it could be in relation to food. This resource from the NHS can help identify common rashes: Rashes in Babies and Children
Signs it might not be contact irritation and actually a food allergy:
- The rash spreads and is widespread and is raised or hives (often appears quickly within a few minutes and looks similar to a ‘nettle sting’ with raised white weals).
- The rash is getting worse and is in combination with other symptoms such as lip or eye swelling, vomiting or diarrhoea
- In severe cases causing breathing difficulties, persistent coughing or going tired or floppy (all symptoms of anaphylaxis) seek immediate medical help and call 999. Anaphylaxis is rare in little ones but can happen.
Check out Charlotte’s blog “Is my baby’s rash a food allergy?”
Useful tip!
Taking photos or videos at the time of suspected reaction can be useful to present to your Healthcare Professional (HCP) and is easier for them to identify the severity of the reaction rather than a description.

My baby has had a reaction to peanut or another allergen, what should I do?
For peanut, reactions are mostly likely IgE mediated (immediate) and typically present within the first 30 minutes.
If your baby has had an immediate reaction and this has not happened before, please seek immediate medical support. For mild- moderate reactions call 111 or speak with your GP. For severe reactions call 999.

Further information on the difference between mild- moderate and severe reactions can be seen below and in the BSACI infant feeding guide for parents factsheet.
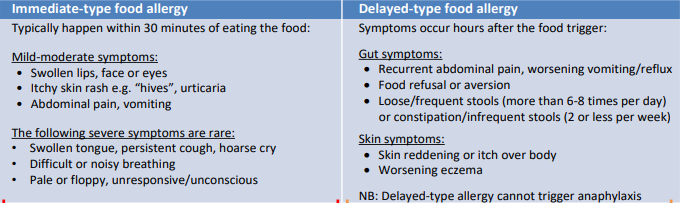
Reproduced from BSACI Infant Feeding Guide For Parents.
Should I consult my GP?
Whether you are suspecting an allergy or not, it’s important to consult with your GP if your baby has a reaction to a food.
Your GP will listen to your concerns and will ask you specific questions (also referred to as an allergy focused history).
This will include questions such as:
- Family history (such as if you or other family members have eczema, asthma, hay fever or food allergy)
- Atopy of baby (such as eczema). Atopy refers to the genetic tendency to develop allergic diseases. Having eczema particularly if it is severe and early onset (within the first few months of life) is a risk factor for developing food allergy.
- Feeding history & growth
- Previous management such as eczema (e.g. not responding to emollient or steroid) or not responding to reflux medication.
- Symptoms including:
- Type (IgE or non IgE mediated)
- Age of baby
- Severity of symptoms
- Amount eaten and in what form (e.g a teaspoon of scrambled egg)
- Reproducibility of symptoms (have the symptoms appeared before if there has been repeated exposure?)
From here, if appropriate your GP will consider a referral to the local allergy clinic.
Typically for mild-moderate non IgE mediated (delayed) allergies these are managed in the community with your GP or other HCP but this will vary across different areas and resources available.
What to ask your GP
Once your GP has gone through an allergy focused history, they will then discuss the next appropriate steps with you. You may also want to consider the following questions to ask…
- Can my baby be referred into a local allergy service?
- Can my baby be referred to a dietitian?
- What do I do if this allergic reaction happens again? When do I need to worry?
- Does my baby need any allergy medication?
Feel free to add other questions to this list.
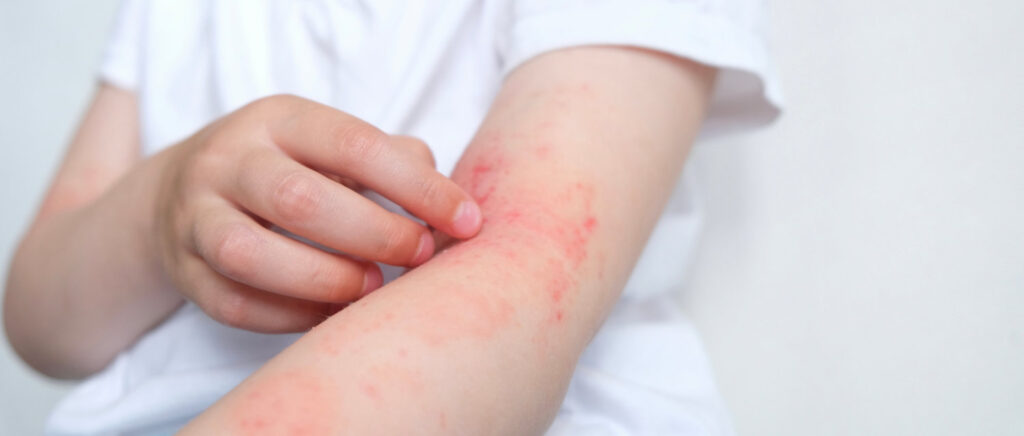
If my baby has a reaction, should I avoid all common allergens?
This is a question that crops up regularly in clinic. Understandably, the thought of introducing other allergens after a reaction can be anxiety provoking which is why discussing further with an Allergist and allergy dietitian is advised to discuss the best approach for your baby.
It is, however, important not to delay other allergens, we have good research and guidance to include common allergens into your baby’s diet before 12 months of age to help prevent food allergies. Particularly food allergens such as egg and peanut. Further guidance can be found here: BSACI
Should we try the food again or leave it until seen by a specialist?
This will depend on the type of reaction your baby has had. Typically, in mild-moderate non IgE mediated (delayed) allergy, if you are unsure if your baby has had a reaction, it is safe to consider trialling again at home as although symptoms are uncomfortable, they are not life threatening.
If you are unsure if your baby is having a mild-moderate non IgE mediated (delayed) reaction, stop the suspected food and wait for symptoms to resolve and look to re trial in 1-2 weeks. If symptoms return this means it’s more likely allergy and you need to discuss further with your GP or HCP.
For suspected IgE mediated (immediate) allergies, this needs to be discussed on an individual basis with your HCP and to avoid that specific food until advice has been sought.
What if my specialist appointment is in 6 months
Unfortunately, in the current climate long waiting times are common and access to specialist appointments can take some time. It is worth finding out if you have been referred to a dietitian as they can support you while waiting.
If you are still struggling to get the support you need, patient organisations such as Allergy UK and BSACI have information on their website to support weaning and allergic reactions as well as the Allergy UK helpline. Allergy UK also have a fantastic factsheet that should help you here.
Huge thank you to Lydia Collins-Hussey, The Milk Allergy Dietitian is a Specialist Paediatric Allergy Dietitian for writing this blog.
Lydia has over 10 years’ experience in the NHS and private practice and her passion is helping families cut through the nutrition noise so that they feel confident feeding their baby. Lydia has her own private practice http://www.themilkallergydietitian.com and Instagram @themilkallergydietitian.
