Iron is a mineral and an important component of a healthy, balanced diet in babies, children and adults. But, do we really understand how much iron we should be getting during pregnancy, and how much babies should be having in the early years of life?
Now I know there can be a lot of confusion around this topic, so in this article I’ll look at WHY pregnant women and babies need iron, how much is needed and how both expectant mums and babies can get enough iron from a healthy diet.
Why do we need iron?
Iron is a micronutrient that helps to make red blood cells which are responsible for transporting oxygen around the body. It also aids in the normal function of the immune system.
Iron deficiency (when we have an insufficient supply of iron) or iron deficiency anaemia (where the body can’t produce enough red blood cells due to really low iron stores) may cause a variety of complications in the body which include symptoms such as tiredness, shortness of breath, heart palpitations and headaches.
Children can be at higher risk of iron deficiency and, as well as the above symptoms, there may be long term implications on brain function as a result of iron deficiency anaemia.
The latest results from the National Diet and Nutrition Survey highlight iron as a nutrient of particular concern for young children. This is due to the fact that around 11% of young children were shown to have very low iron intakes in the latest studies. Some children are at risk of anaemia as a result of low intakes of iron. Latest estimates are that 30% of 1.5-3 y have iron deficiency (low iron stores) and 5% may have anaemia.

How much iron do I need during pregnancy?
Pregnant women need more iron in their bodies due to their bodies and bump growing and needing a good supply of blood and oxygen to do so. Additionally pregnant women are growing a new human – creating new cells and a new person which is in itself growing day by day too. All of this needs oxygen and iron plays an important role in transporting oxygen around the body.
Additionally research has shown that iron levels at birth determine a baby’s iron levels throughout infancy. In other words, the iron you supply your baby with throughout your pregnancy will be incredibly important to your baby’s overall iron levels after birth and into their early months. So it’s important for pregnant women to maintain a good supply of iron.
However, interestingly in the UK the recommended amounts of iron to have during pregnancy are the same as those of non-pregnant women at around 14.8mg/day. This isn’t because pregnancy and growing a baby doesn’t require more iron, but simply because the human body is very clever and during pregnancy it adapts to maintain higher iron levels. Therefore, most people need to get enough iron, but they don’t need to eat extra or take supplements to try and achieve this.
Do I need an iron supplement during pregnancy?
In the UK we don’t recommend that women take a routine iron supplement during pregnancy. Supplementation is ONLY recommended if women have low iron in their blood during the first trimester or at 28 weeks.
Yet, approximately 20% of pregnant women suffer with iron deficiency anaemia so it’s a good idea to become familiar with how much iron you need and exactly where you can get it in the diet! Have a chat with your midwife or GP if you’re not sure and see if they can check your levels via a blood test.

How much iron does my baby need?
Provided baby is born on time with a healthy birth weight and mum had decent iron stores during pregnancy, babies should be born with the correct iron supplies that they need for the first 6 months of life. Therefore breastmilk and/or formula are the only food your baby needs during this time.
From (around) 6 months onwards, breast milk and/or fortified formula are no longer sufficient alone to meet the increasing iron requirements, and infants will need to begin to receive iron from a range of other dietary sources.
Table 1 below, adapted from The British Dietetic Association, breaks down the iron recommendations for infants and children.
Adapted from: BDA Food Fact Sheet
Do babies need iron supplements?
Aside from vitamins A, C & D, there are no nutrients which are recommended to be supplemented for ALL babies and children. The best way to ensure that your little one (after 6 months) is getting all of the nutrients they need, is to offer a balanced diet with a variety of foods.
In certain situations your healthcare provider (HCP) or GP may recommend a supplement containing iron, and there are some dietary restrictions that might call for extra vitamins and minerals in the diet of young children. Speak to your HCP about this and check out my article on supplements for babies and young children to read more.
Do babies need iron supplements?
Iron is available in two forms – we have plant-based iron (called non-haem iron) and animal-based iron (called haem iron).
Haem iron is the easiest type of iron for our and our babies’ bodies to absorb and effectively use. We can acquire haem iron from a variety of animal products such as red meats, pork, fish and liver (FYI, liver and pate are NOT suitable for babies under one or pregnant women). You might find my articles on how to introduce meat to your baby and fish recommendations for babies useful.
Non-haem iron can be found in foods such as broccoli, beans, lentils, tofu, cereals and ground nuts. Our bodies find it a little bit more difficult to absorb iron from non-haem sources therefore it is recommended that we may need to eat a little more of these foods if we’re not eating any meat or haem iron. It’s also good to have a variety of non-haem sources and lastly it may be helpful to have a source of vitamin C alongside iron-rich foods, as this can help enhance the absorption of iron from non-haem sources.
Here are a few examples of how to combine iron rich foods with vitamin C:
- A handful of berries with fortified-cereal at breakfast
- Slices of chopped pepper with a sandwich at lunch
- Having a few slices of orange or kiwi alongside dinner
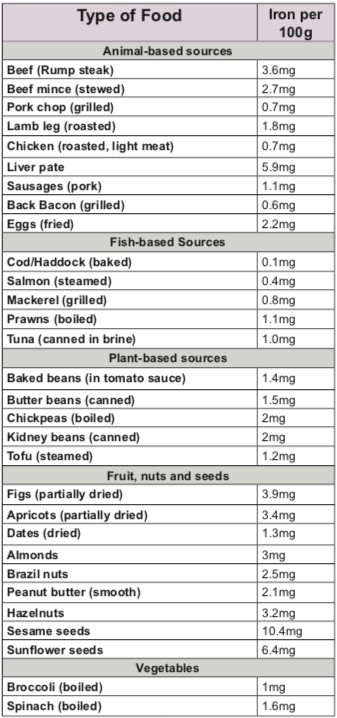
See Table 2 below which shows the iron content of different food sources. Why not screenshot this and use this when you plan your weekly menu!
Table 2, taken from: BDA Food Fact Sheet
N.B liver and pate are NOT suitable for babies under one or pregnant women due to the high content of vitamin A in them.)
Take home points:
- Pregnant women have higher iron needs than non-pregnant women, but most of this can be obtained from a well-balanced diet and including 2-3 portions of iron rich foods. Pregnant women also play a vital role in preventing their baby from developing low iron stores at birth.
- From 6 months onwards, infants need to eat a variety of foods including some which are good sources of iron to meet the increasing micronutrient demands of a growing baby.
- Including 2-3 portions of iron rich foods (variety helps too) in pregnant women’s diets as well as young children once they are established onto solids will help ensure they are getting enough.
I hope you found this post interesting and thank you for reading! I post lots about baby and child nutrition over on Instagram, so do join me there if you’d like to read more.
(N.B liver and pate are NOT suitable for babies under one or pregnant women due to the high content of vitamin A in them.)


Further Reading:
Government Dietary Recommendations:
SACN report “Feeding in the First Year of Life”:
https://www.gov.uk/government/news/sacn-publishes-feeding-in-the-first-year-of-life-report
SACN paper on iron:
https://www.gov.uk/government/publications/sacn-iron-and-health-report
Article first written by Holly Roper MSc student University of Sheffield with support from SR Nutrition.
Later adapted by Katarina Martinez-Thomas for SR Nutrition.

Charlotte’s Book!
